Connect With Us
Blogs

How to Care for Your Arthritic Foot
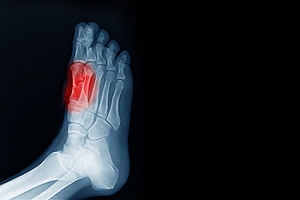
Arthritis is an inflammation of the joints and it can occur at any joint in the body, especially in the foot. It generally effects those who are older, however, it can occur at any age. Although there are many different forms of arthritis, there are three main types that occur in the foot. The three types are osteoarthritis, rheumatoid arthritis, and gout.
The primary cause of osteoarthritis is aging. As you age, cartilage degenerates around the joints which causes friction and pain. Obesity can cause osteoarthritis through mechanical stress. Injuries that damage joints can increase the probability as well. Finally, a family history of osteoarthritis can also increase chances of having it.
Rheumatoid arthritis occurs when the immune system attacks the joint linings and weakens them over a long time. While there is no known cause of rheumatoid arthritis, obesity and smoking can increase your chances of getting it. Women are also more likely to get it than men.
Gout is a form of arthritis that occurs when there is too much uric acid in your blood and painful crystals form in your joints. Men are more likely to have gout than women. People who are obese or drink alcohol often are also more likely to develop gout. Furthermore, having diabetes, heart disease, high blood pressure, high cholesterol, gastric bypass surgery or a family history of gout may increase your likelihood of developing the condition.
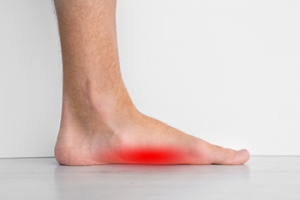
Symptoms of arthritis include pain, stiffness, swelling in the joints. These symptoms can make it harder and more painful to walk. Physical activity can increase pain and discomfort. Furthermore, joint pain can worsen throughout the day for osteoarthritis. Gout attacks generally last several days with the first few being the worst.
Diagnosis of gout includes either a joint fluid test or a blood test. X-ray imaging can detect osteoarthritis but not gout. On the other hand, there is no blood test for osteoarthritis. Rheumatoid arthritis is difficult to diagnosis. Doctors utilize family and personal medical history, a physical examination, and antibody blood tests to determine if you have rheumatoid arthritis.
Treatment varies for the different kinds of arthritis. Anti-inflammatory medication or steroids can help reduce pain from inflammation of the joints. Changing shoe types can help with some symptoms. Wider shoes can help with discomfort from gout and osteoarthritis. High heels should be avoided. Shoes with proper arch support and that take pressure off the ball of the foot can help with rheumatoid arthritis. Drinking lots of water can also help rid uric acid from the blood. Losing weight, improving your diet, and limiting alcohol and smoking can also help prevent or lessen the symptoms of arthritis.
If you are having trouble walking or pain in your feet, see a podiatrist to check if you have arthritis.
Effective Stretches for Runners

Runners can benefit greatly from incorporating specific stretches into their routine to enhance flexibility and prevent injury. The knee hug is an effective stretch that targets the glutes and lower back. By pulling one knee towards the chest while standing, runners can alleviate tension and improve hip mobility. Another beneficial stretch is the child’s pose, which stretches the lower back, hips, and thighs. To perform this stretch, kneel on the floor, extend your arms forward, and lower your torso towards the ground. The standing quad stretch helps maintain flexibility in the quadriceps and hip flexors. By grabbing one ankle and gently pulling it towards the glutes while standing, runners can effectively stretch these key muscle groups. If you have suffered a foot or ankle injury while running, it is suggested that you visit a podiatrist to treat your specific foot condition and guide you on effective running injury prevention methods.
All runners should take extra precaution when trying to avoid injury. If you have any concerns about your feet, contact one of our podiatrists of Granite State Podiatry Associates. Our doctors will treat your foot and ankle needs.
How to Prevent Running Injuries
There are a lot of mistakes a runner can make prior to a workout that can induce injury. A lot of athletes tend to overstretch before running, instead of saving those workouts for a post-run routine. Deep lunges and hand-to-toe hamstring pulls should be performed after a workout instead of during a warmup. Another common mistake is jumping into an intense routine before your body is physically prepared for it. You should try to ease your way into long-distance running instead of forcing yourself to rush into it.
More Tips for Preventing Injury
- Incorporate Strength Training into Workouts - This will help improve the body’s overall athleticism
- Improve and Maintain Your Flexibility – Stretching everyday will help improve overall performance
- “Warm Up” Before Running and “Cool Down” Afterward – A warm up of 5-10 minutes helps get rid of lactic acid in the muscles and prevents delayed muscle soreness
- Cross-Training is Crucial
- Wear Proper Running Shoes
- Have a Formal Gait Analysis – Poor biomechanics can easily cause injury
If you have any questions, please feel free to contact our offices located in Manchester and Bedford, NH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Preventing Running Injuries
Over half of all runners encounter at least one injury per year. The reason for this is because many runners do not train properly. Injuries are almost inevitable due to the physical stress that running causes. While our bodies are great at adapting to the stress, it can only handle it in small doses. Injuries occur when the stress is applied too quickly for the body to handle, causing something within it to break down. With each step you take, your leg is absorbing two or three times your body’s weight.
Some of the most popular running injuries are shin splints, plantar fasciitis, Achilles tendinitis, and stress fractures. Shin splints cause pain along the inside or outside of the shins, and this pain is usually felt at the beginning of a run. The condition itself is defined as an inflammation of the muscles or tendons located around the shinbone. To treat shin splints, it is advised that you ice the shin area and stretch the calf muscles. To prevent this injury, you should slowly increase the distance you plan on running, instead of jumping into a more strenuous routine.
Achilles tendinitis is another common injury and it feels like pain along the back of the leg, toward the heel. This condition is defined as an inflammation of the Achilles which is the largest tendon in the body. The Achilles is responsible for connecting your calf muscles to the heel bone and it is caused by tight calf muscles. If you want to treat this injury, you should take a break from running to cross train with a low-impact activity.
There are a lot of common mistakes runners make that are causing them to experience injury. One mistake is stretching too much prior to warming up. If you plan to go on a run, you should warm up with a gentle 3-5-minute walk followed by a 5-minute run-walk. Another common mistake is jumping into a routine too quickly. Consequently, you should incorporate cross-training into your routine. If you are looking to get active, you should slowly weave running into an activity you are currently participating in. For example, you can try bike riding for 40 minutes followed by a 10-minute run.
Another way to prevent running injuries is to choose shoes that are appropriate for running. There are certain things you should look for when buying a new pair of running shoes. An important factor in these sneakers is flexibility. Running shoes should be capable of bending and flexing at the forefoot. However, you should not be able to bend the entire shoe in half with ease because this is a sign that the shoe does not have enough structure. Additionally, you should look for the fit of the running shoes you want to purchase. It is best to visit a specialty running shoe store to have your feet properly sized. Choosing shoes that fit properly can prevent many foot ailments.
If you are suffering from any pain from running injuries, you should make an appointment with your podiatrist to discover the underlying cause of your pain. He or she will be able to help treat your condition in the best way possible.
Identifying and Treating Sesamoiditis
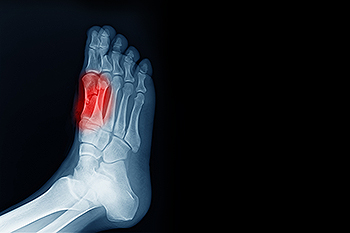
Sesamoiditis is an irritation of the two sesamoid bones that are located beneath the first metatarsal head of the foot. It leads to pain that can be particularly bothersome during activities like walking or running. These tiny bones, each about the size of a kernel of corn, play a significant role in foot movement. They can become painful due to trauma, foot structure changes, or repetitive stress. Sesamoiditis is often seen in dancers, runners, and those who frequently wear high heels. Symptoms can include localized pain beneath the big toe, swelling, and tenderness that worsens with pressure. Diagnosis typically involves a clinical evaluation by a podiatrist, sometimes supported by imaging tests to rule out fractures or other conditions. Treatment focuses on reducing pressure on the sesamoids through footwear modifications, including supportive shoes and custom orthotics. If you have pain under the big toe, it may be related to the sesamoid bones, and it is suggested that you schedule an appointment with a podiatrist for an exam and treatment.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact one of our podiatrists of Granite State Podiatry Associates. Our doctors will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
- Sudden increase in activity
- Increase in physically strenuous movement without a proper warm up or build up
- Foot structure: those who have smaller, bonier feet or those with a high arch may be more susceptible
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions please feel free to contact our offices located in Manchester and Bedford, NH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sesamoiditis
Sesamoiditis is a condition in which the sesamoid bones in the forefoot become inflamed from physical activity. Sesamoid bones are bones that are not connected to other bones but are located in tendons or muscle. Two of these sesamoid bones are very small and located on the underside of the foot near the big toe. Athletes such as runners, baseball and football players, and dancers are likely to experience sesamoiditis. Those with high arched feet, flat feet, or runners who run on the ball of their foot are also prone to suffer from sesamoiditis.
Symptoms include pain or throbbing on the ball of the foot near the big toe. The pain generally starts with a mild throbbing but gradually builds up to shooting pain. Bruising, swelling, and redness are possible, but in most cases, these symptoms are not present. However, moving the big toe can result in pain and difficulty.
To conduct a diagnosis, the podiatrist will examine the ball of the foot and big toe. They will look for any outliers and check the movement of the toe. X-rays will be taken to rule out any other conditions and ensure that it is sesamoiditis.
Treatment for sesamoiditis is generally mild and includes rest, anti-inflammatory and pain medication, and ice treatments to deal with the swelling and pain. Orthotics may be needed with people who have flat or high arched feet to relieve pressure off the bones. In some cases the toe will be taped and immobilized to allow healing. The podiatrist may also decide to use a steroid injection to help with swelling as well. If you have sesamoiditis, you shouldn’t engage in any intensive activity, as it may inflame the area and worsen your pain. If the sesamoid bone has fractured, surgery may be required to remove the sesamoid bone.
If you are suffering from sesamoiditis or are experiencing symptoms similar to sesamoiditis, you should stop all physical activity that puts strain on the area. Furthermore you should see a podiatrist for a diagnosis to see if you have sesamoiditis.
Impacts of Flat Feet on All Ages
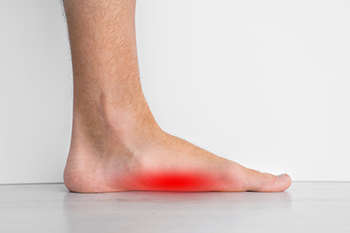
Flat feet, or fallen arches, occur when the arch of the foot collapses, leading to the entire foot making contact with the ground. Symptoms can include foot pain, swelling, and difficulty standing for long periods of time. Causes can range from genetic factors to injury or conditions such as arthritis. In children, flat feet are often a normal part of development, usually improving with age. However, if persistent, they may require intervention. In adults, flat feet can result from wear and tear, obesity, or excessive strain. Both children and adults may experience discomfort or difficulty in activities. Treatment options include wearing supportive footwear, using orthotics, and doing exercises to strengthen the foot muscles. If you or your child has flat feet, it is suggested that a podiatrist is consulted and regular visits are scheduled to help manage this condition.
Flatfoot is a condition many people suffer from. If you have flat feet, contact one of our podiatrists from Granite State Podiatry Associates. Our doctors will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our offices located in Manchester and Bedford, NH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flatfoot
Flatfoot is a foot disorder that is not as straightforward as many people believe. Various types of flatfoot exist, each with their own varying deformities and symptoms. The partial or total collapse of the arch, however, is a characteristic common to all types of flatfoot. Other signs of flatfoot include:
- “Toe drift,” or the pointing outward of the toes and the front part of the foot
- The tilting outward of the heel and the tilting inward of the ankle
- The lifting of the heel off the ground earlier when walking due to a tight Achilles tendon
- Hammertoes
- Bunions
One of the most common types of flatfoot is flexible flatfoot. This variation usually starts in childhood and progresses as one ages into adulthood. Flexible flatfoot presents as a foot that is flat when standing, or weight-bearing. When not standing, the arch returns. Symptoms of flexible flatfoot include:
- Pain located in the heel, arch, ankle, or along the outside of the foot
- Overpronation, or an ankle that rolls in
- Shin splint, or pain along the shin bone
- General foot aches or fatigue
- Pain located in the lower back, hip, or knee
Your podiatrist will most likely diagnose flatfoot by examining your feet when you stand and sit. X-rays may be taken to define the severity and help determine the treatment option best for your condition. Nonsurgical treatments can include activity modification, weight loss, orthotics, immobilization, medications, physical therapy, shoe modifications, and ankle foot orthoses (AFO) devices. If nonsurgical methods prove ineffective, surgery may be considered. Multiple surgical procedures can correct flatfoot; and depending on your specific condition, one may be selected alone or combined with other techniques to ensure optimal results.
Arthritis Can Cause Pain in the Feet and Ankles
Heel Pad Syndrome
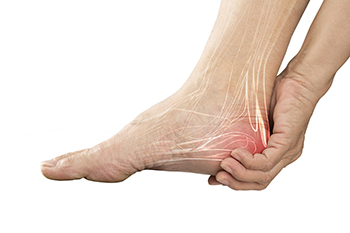 Heel pad syndrome is a painful condition affecting the heel's fatty tissue, leading to discomfort and difficulty walking. This syndrome occurs when the heel's fat pad, which acts as a shock absorber, deteriorates or thins out, often due to excessive stress or injury. The condition can result from aging, repetitive high-impact activities like running or jumping, prolonged standing, or being overweight. Heel pad syndrome can affect anyone but is more common among athletes, older adults, and individuals with occupations requiring extended periods of time on their feet. Symptoms typically include a deep, bruised feeling in the heel, particularly noticeable during weight-bearing activities. This pain can be sharp or aching, worsening with activity and improving with rest. If you have painful heels, it is suggested that you schedule an appointment with a podiatrist who may prescribe orthotics, heel cups, specific exercises, and anti-inflammatory medication.
Heel pad syndrome is a painful condition affecting the heel's fatty tissue, leading to discomfort and difficulty walking. This syndrome occurs when the heel's fat pad, which acts as a shock absorber, deteriorates or thins out, often due to excessive stress or injury. The condition can result from aging, repetitive high-impact activities like running or jumping, prolonged standing, or being overweight. Heel pad syndrome can affect anyone but is more common among athletes, older adults, and individuals with occupations requiring extended periods of time on their feet. Symptoms typically include a deep, bruised feeling in the heel, particularly noticeable during weight-bearing activities. This pain can be sharp or aching, worsening with activity and improving with rest. If you have painful heels, it is suggested that you schedule an appointment with a podiatrist who may prescribe orthotics, heel cups, specific exercises, and anti-inflammatory medication.
Many people suffer from bouts of heel pain. For more information, contact one of our podiatrists of Granite State Podiatry Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Manchester and Bedford, NH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.